
Rev. Ciencias Veterinarias, Vol. 43, N° 1, [1-12], E-ISSN: 2215-4507, enero-junio, 2025
DOI: https://doi.org/10.15359/rcv.43-1.3
URL: http://www.revistas.una.ac.cr/index.php/veterinaria/index
Eumycetoma caused by Fonsecaea sp.: case report of a cat in Costa Rica
Reporte de caso de eumicetoma por Fonsecaea sp. en un felino doméstico de Costa Rica
Relato de caso de eumicetoma por Fonsecaea sp. em um felino doméstico de Costa Rica
Ericka Diez-Guevara1,2, Ricardo García-Rodríguez1,3, Alejandra Calderón-Hernández4
1 Veterinary Cytology Division, Vetlab Laboratory, San José, Costa Rica. rigarod@gmail.com,
 https://orcid.org/0009-0002-2862-9970
https://orcid.org/0009-0002-2862-9970
2 Oftalvet, Dr. Pets Veterinary Center, San José, Costa Rica. erickadiezg@gmail.com,
 https://orcid.org/0009-0004-9940-3068
https://orcid.org/0009-0004-9940-3068
3 García & Pérez Veterinary Clinic, San José, Costa Rica.
4 Mycology Laboratory, School of Veterinary Medicine, Universidad Nacional, Heredia, Costa Rica. *alejandra.calderon.hernandez@una.ac.cr,  https://orcid.org/0000-0002-7031-5193
https://orcid.org/0000-0002-7031-5193
 Corresponding author: alejandra.calderon.hernandez@una.ac.cr
Corresponding author: alejandra.calderon.hernandez@una.ac.cr
Received: February 2, 2025. Corrected: June 10, 2025. Accepted: June 12, 2025
Although subcutaneous mycoses are not common, they are more frequent in domestic cats due to behaviors such as burying feces, hunting, and engaging in territorial disputes. However, these pathologies are often underdiagnosed because their clinical signs can be confused with tumoral or bacterial etiologies. This paper reports the first case of eumycetoma caused by Fonsecaea sp. in a cat. In late September 2018, an 8-year-old male mixed-breed feline was treated for a suppurative lesion on the nasal plane, with a recent history of squamous cell carcinoma in the left ear, which had been treated with a conchectomy. During the clinical examination, the cat was found to have a poor body condition score of 2/5. The nasal lesion resulted in sneezing, experiencing pain, and having swollen mandibular lymph nodes. The lesion appeared inflamed and exhibited fistulous characteristics, with black granules and serosanguineous drainage. The cat tested negative for feline immunodeficiency virus and feline leukemia virus, and radiographs of the head revealed bone lysis. Fine-needle aspiration cytology revealed the presence of granular dematiaceous thalli, confirming a diagnosis of eumycetoma. Fonsecaea sp. was identified through mycological culture. The patient was treated with Itraconazole 50 mg PO SID for one month but later developed neurological signs and was euthanized. Due to the recurrent and invasive nature of dark fungi and their poor response to antifungals, a mycological culture is always recommended whenever a mycosis is suspected or confirmed to ensure more effective management of these pathologies.
Keywords: subcutaneous mycosis, dematiaceous fungus, cytology, itraconazole.
Resumen
Las micosis subcutáneas son infrecuentes, pero se reportan más en los felinos domésticos debido a su forma de vida: entierran las heces, cazan, pelean por territorio, entre otras. No obstante, se consideran subdiagnosticadas, debido a que su presentación clínica se confunde con patologías de origen tumoral o bacteriano. El objetivo de este trabajo es informar sobre el primer caso de eumicetoma por Fonsecaea sp. en un gato. A finales de septiembre de 2018, se atiende a un felino, macho, sin raza definida, de aproximadamente 8 años, por motivo de una lesión supurativa en el plano nasal, con historia reciente de carcinoma de células escamosas en la oreja izquierda que se trató mediante conquectomía. El examen objetivo general presentaba una condición corporal baja de 2/5. La lesión le ocasionaba estornudos, dolor y presentaba los nódulos linfáticos mandibulares aumentados, se notaba inflamada y fistulosa con drenaje de gránulos negros en un material serosanguinolento. El gato resultó negativo para los virus de inmunodeficiencia felina y leucemia felina, además, la radiografía de cabeza indicó lisis ósea. Se realizó una citología por aspiración con aguja fina donde se observaron talos en grano dematiáceos, con lo cual se obtuvo un diagnóstico de eumicetoma. En el cultivo micológico se identificó Fonsecaea sp. Se trató con itraconazol 50 mg PO SID durante un mes, hasta que desarrolló sinología nerviosa y se le practicó eutanasia. Debido al carácter recidivante, invasivo y escasamente responsivo de los hongos negros a los antifúngicos, se recomienda realizar siempre cultivo micológico cuando se sospecha o se confirma una micosis para un mejor manejo de estas patologías.
Palabras clave: micosis subcutánea, hongo dematiáceo, citología, itraconazol.
Resumo
As micoses subcutâneas são infrequentes, mas são mais relatadas em felinos domésticos devido ao seu estilo de vida: enterram fezes, caçam, brigam por território, entre outros. No entanto, são consideradas subdiagnosticadas, pois sua apresentação clínica pode ser confundida com patologias de origem tumoral ou bacteriana. O objetivo deste trabalho é relatar o primeiro caso de eumicetoma por Fonsecaea sp. em um gato. No final de setembro de 2018, foi atendido um felino, macho, sem raça definida, de aproximadamente 8 anos, com uma lesão supurativa na região nasal, com histórico recente de carcinoma de células escamosas na orelha esquerda, tratado por conqueotomia. No exame físico geral, apresentava condição corporal baixa, 2/5. A lesão causava espirros, dor e aumento dos nódulos linfáticos mandibulares, além de estar inflamada e fistulosa, com drenagem de grânulos negros em material serossanguinolento. O gato testou negativo para os vírus da imunodeficiência felina e leucemia felina. A radiografia de crânio indicou lise óssea. Foi realizada uma citologia por punção aspirativa por agulha fina, na qual se observaram talos em grânulos demáceos, permitindo o diagnóstico de eumicetoma. No cultivo micológico foi identificado Fonsecaea sp. O tratamento foi feito com itraconazol 50 mg VO SID durante um mês, até que o animal desenvolveu sinais neurológicos e foi submetido à eutanásia. Devido ao caráter recorrente, invasivo e à baixa responsividade dos fungos negros aos antifúngicos, recomenda-se sempre realizar cultivo micológico quando houver suspeita ou confirmação de micose, para um melhor manejo dessas patologias.
Palavras-chave: micose subcutânea, fungo demáceo, citologia, itraconazol.
Subcutaneous mycoses are more common in felines than in canines (Seyedmousavi et al., 2013), likely due to their unique behavior as outdoor cats, which exposes them to injuries from barbed wire, fences, or other sharp materials. Burying feces with their limbs makes them susceptible to accumulating large amounts of organic matter and fungal conidia in their claws, which would later be implanted in the subcutaneous tissue because of fights for territory, mating, or self-trauma. At the same time, they are prone to suffering lacerations because of their hunting behavior (Loyd et al., 2013; Overall, 2013).
Implantation of fungal diseases in cats are primarily found in the facial region, the nasal bridge, and the distal part of the extremities or tail. The appearance is soft and mobile, with painless nodules of variable consistency. Their content may be serosanguineous or contain reddish, black, or dark brown granules, resulting in pigmentation of the affected area. These lesions may ulcerate, fistulate, or form crusts and become complicated by the growth of other microorganisms. Additionally, the nodules may be non-ulcerated, subcutaneous, or plaque-like, and can be either focal or multifocal, with local invasion. Depending on the fungus involved, there may be invasion of nearby tissues or systemic dissemination, causing variable signs (Grooters, 2021; Lloret et al., 2013).
Fungal etiology depends on the local epidemiology, with infections more commonly caused in the tropics by dematiaceous fungi (black or pigmented) (Rodrigues & Albuquerque, 2018). However, a notable number of cases of phaeohyphomycosis have been reported in the United Kingdom, caused by Alternaria spp., and in Australia caused by Microsphaeropsis arundinis (Barrs et al., 2024).
Dematiaceous subcutaneous fungal infections are clinically very similar and are characterized by a painless onset and slow progression (months to even years). Although very similar, three of these infections —phaeohyphomycosis, eumycetoma, and chromoblastomycosis —differ in their anatomical location, etiology, and the way the fungus adapts to the tissue (Arenas & Torres, 2019; Bonifaz-Trujillo, 2020).
Septate dematiaceous hyphae, accompanied by the presence of pseudomycelia and/or blastospores, are the adaptation found in phaeohyphomycosis. Most cases have occurred in felines, generally on the head or distal extremities (Grooters, 2021). In some cases, more specifically diseases caused by Curvularia spicifera (formerly Bipolaris spicifera) or Exserohilum rostratum, have been accidentally categorized as eumycetomas (Pohlman & Chengappa, 2022).
The presence of grains or grain-shaped thalli (microcolonies) of filamentous fungi, whether pigmented or hyaline, is indicative of eumycetoma. In contrast, when these are caused by filamentous bacteria belonging to the order Actinomycetales, they are categorized as actinomycetoma (Arenas & Torres, 2019; Bonifaz-Trujillo, 2020). The latter are more frequent in felines, while eumycetoma is rare in domestic animals but occasionally occurs in cats, horses, and canines (Pohlman & Chengappa, 2022; Seyedmousavi et al., 2013).
Finally, sclerotic cells or Medlar bodies are the structures found in samples positive for chromoblastomycosis (Seyedmousavi et al., 2013; Seyedmousavi et al., 2018; Westblade et al., 2023), which is a disease that occurs mainly in humans, and, in the case of animals, it has only been reported in amphibians (Seyedmousavi et al., 2018).
Due to the limited number of reports on eumycetoma in animals, this study aims to increase awareness within the veterinary community about this fungal infection, emphasizing its importance in the differential diagnosis of nodular lesions in cats.
On June 4, 2018 (Day 1), an approximately 8-year-old, neutered, mixed-breed, domestic, male feline was rescued from the streets and taken to a veterinary clinic in Curridabat, San José, Costa Rica, in an emaciated state with two skin lesions. Upon clinical examination, the patient weighed 2.85 kg and had a poor body condition (score of 2/5). There was inflammation over the nasal plane, in addition to an extensive lesion on the left ear that covered the auricle on its external and internal sides (Figure 1). During this consultation, the animal was dewormed, and an automated blood test revealed mild non-regenerative anemia (hematocrit 18.8 %, range [24-45] %, hemoglobin 5.9 g/dl, range [8.0-15.0] g/dl) and an inflammatory response (leukocytosis 30.9 x 109 /L, range [5-18.9] x 109 /L). In addition, the tests for feline immunodeficiency virus and feline leukemia virus were negative.

Figure 1. Day 1: inflammation over the nasal plane (circle) and a nodular ulcerative lesion on the left ear covering the edge and posterior part.
On day 14, renal and hepatic blood biochemistry revealed a slight increase in globulins (55 g/L, range [28-51] g/L) and a slight decrease in albumin (20 g/L, range [22-40] g/L). In addition, lesions were evaluated and x-rayed, showing an overgrowth of soft tissue in the nasal plane.
On day 18, a cytology of the nasal planum revealed a pyogranulomatous inflammation of possible fungal origin, maybe caused by pigmented fungi caused by pigmented fungi. Based on this result, treatment was initiated with oral itraconazole at 10 mg/kg every 12 hours for one month; however, no clinical improvement was observed during treatment.
On day 37, a conchectomy was performed on the patient’s left ear due to the extent of the lesion, and the tissue was sent for histopathological examination. The pre-surgical blood count indicated mild anemia (hematocrit 23.7 %, range [24-45] %, hemoglobin 7.8 g/dL, range [8-15] g/dL).
On day 58, recovery of the hematocrit was detected in the blood control (29.6 %, range [24-45] %).
On day 60, a secondary lesion appeared on the scarred edge of the ear, and the patient was kept under observation.
On day 65, the biopsy result indicated squamous cell carcinoma.
On day 89, a second surgery was performed to remove the new lesion in the area. The patient showed satisfactory improvement in the area, with no new growth.
On day 104 (two months after finishing the itraconazole treatment), an ulcerative wound appeared in the nasal area that released black granules from fistulous tracts (Figure 2).
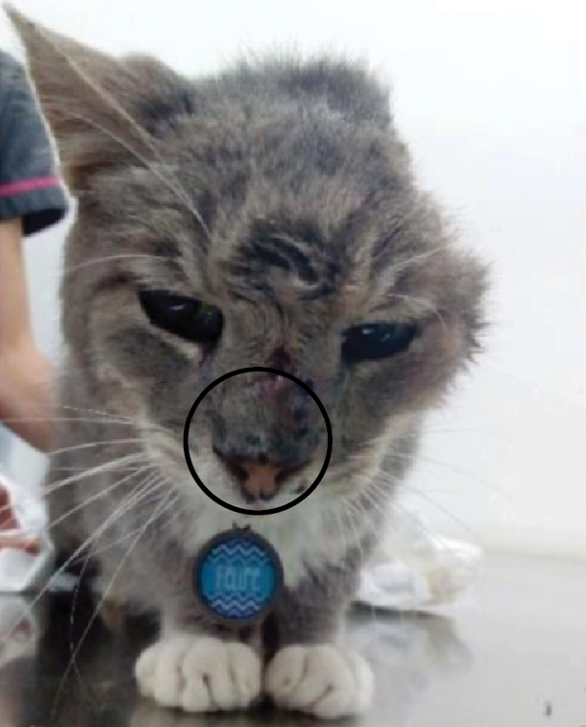
Figure 2. Day 104: suppurative lesion in the nasal plane (circle).
On day 129, the patient was referred to García & Pérez Veterinary Clinic for cytology samples. The patient presented with an inflamed lesion, which drained seropurulent material and black granules at the nasal subcutaneous plane (Figure 3). In addition, the patient also presented local pain, sneezing, and submandibular lymphadenopathy. A fine needle aspiration of the lesion was performed, and five smears were prepared and stained with Wright (Merck KGaA, Darmstadt, Germany). A microscopic examination revealed microcolonies of dematiaceous fungi, characterized by a black, granular thallus (Figure 4), which supports the diagnosis of eumycetoma (Jensen, 2023).
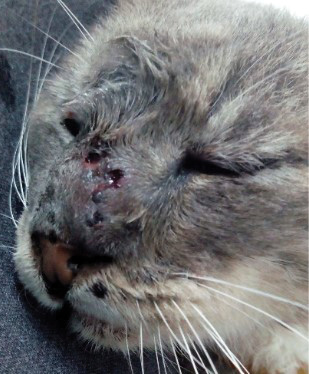
Figure 3. Day 129: suppurative lesion of the nasal plane with fistulas that drain grains (arrows).
__________

Figure 4. Fine needle aspirate cytology showing pyogranulomatous inflammation with a dematiaceous grain-shaped thallus, diagnostic of eumycetoma. Wright, A) 4x and B) 20x.
On day 130, the test for feline immunodeficiency and leukemia was repeated and remained negative.
On day 131, samples for fungal culture were collected by scraping and then swabbing the deep skin lesions and washing the fistulous tracts in the nasal area with sterile saline solution. Direct microscopic examinations were conducted with 40% potassium hydroxide (KOH), Gram stain, and Giemsa stain at the Mycology Laboratory, School of Veterinary Medicine, Universidad Nacional, Costa Rica. At the same time, cultures were performed using Sabouraud Dextrose Agar (Liofilchem, Roseto degli Abruzzi, Teramo, Italy) and Dermasel Agar (Oxoid, Basingstoke, Hampshire, UK) and incubated for three weeks at 28 °C and 37 °C, respectively.
Black grains were macroscopically observed in the swab sample and appeared visible under direct microscopic examination with KOH as filamentous, pigmented microcolonies (dematiaceous grain thalli). Gram staining showed abundant inflammatory cells and dematiaceous septate hyphae, and Giemsa staining showed mixed inflammatory cells and pigmented hyphae. Four colony-forming units (CFU) of a filamentous fungus (18 mm in diameter), dematiaceous on the reverse, dark brown on the front with a velvety texture and a central protrusion were isolated in the three mycological cultures after seven days of growth. This isolate was subcultured on Potato Dextrose agar (Oxoid, Basingstoke, Hampshire, United Kingdom) to induce sporulation (Figure 5). Using an adhesive tape preparation with lactophenol, septate, branched conidiophores with sympodial conidiation and some forming Fonsecaea sp.-type asterisks were observed microscopically. Also, branched conidiophores forming conidia in chains from segments with disjunct tips (shield-shaped cells) as Cladosporium sp.-type and vessel-shaped phialides with cup-shaped collarettes resembling those produced by Phialophora sp. (Figure 6) were seen. The three microscopic morphologies observed allowed the identification of the fungus as Fonsecaea sp. (Arenas & Torres, 2019; Bonifaz-Trujillo, 2020; Westblade et al., 2023).

Figure 5. The macroscopic appearance of the dematiaceous fungus isolated on Dermasel Agar (left) and Potato Dextrose Agar (right) incubated at 28 °C for 14 days.
_______________
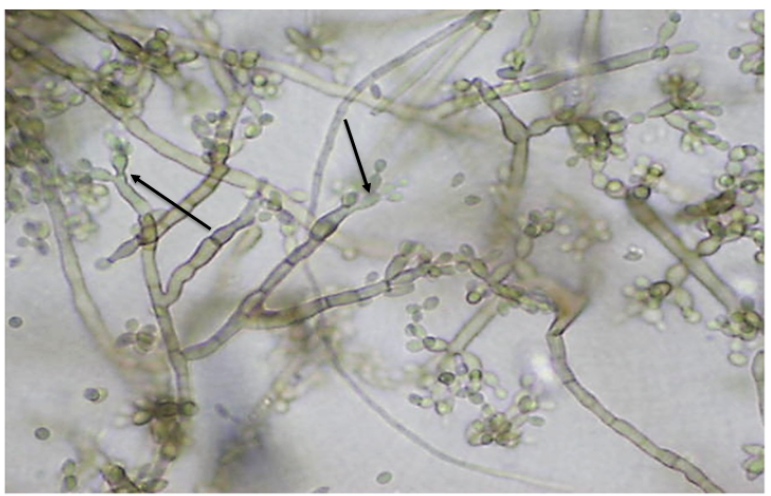
Figure 6. Microscopic appearance of Fonsecaea sp. in lactophenol 40x. Conidiophores with a Fonsecaea-type arrangement (arrows) are observed.
On day 133, the patient began to show signs of weakness, which is why the antifungal treatment was not reinitiated.
On day 136, the first mycology results were received, while the cat continued lethargic with anorexia.
Finally, on day 139, nervous signs began, and humanitarian euthanasia was performed.
Subcutaneous mycoses caused by black fungi in cats from Costa Rica have not been reported. However, the presence of a few cases of phaeohyphomycosis (Calderón-Hernández & Urbina-Villalobos, 2018; Guevara-González, 2022) in the Mycology and Pathology Laboratory of the School of Veterinary Medicine Universidad Nacional, Costa Rica, justifies the importance of conducting this case report.
The clinical signs observed on the patient coincide with what is expected for eumycetoma, especially the presence of granules in the discharge emanating from the skin (Guillot et al., 2004). Tumors and granulomas may appear on the head of domestic felines due to causes such as: trauma, neoplasia, and mainly squamous cell carcinoma (Ferguson, 2012; Barnard, 2013), and causes of infectious origin, such as abscesses caused by Staphylococcus aureus or filamentous bacteria (Barnard, 2013; Ferguson, 2012; Pohlman & Chengappa, 2022), or fungi including Cryptococcus neoformans species complex and Cryptococcus gattii species complex (Singh et al., 2018), Histoplasma capsulatum species complex (Guillot et al., 2018), as well as Sporothrix spp. (Rodrigues et al., 2018), and those fungi that cause eumycetoma and phaeohyphomycosis (Seyedmousavi et al., 2013; Seyedmousavi et al., 2018). Fungal-like algae such as Prototheca spp. are also a rare etiology of these lesions in cats (Sykes, 2021). In addition, parasites such as Leishmania spp. (Baneth et al., 2021; Ferguson, 2012) and Lagochilascaris minor (Solano-Barquero et al., 2022) produce lesions like those presented by fungal etiologies.
In the present case, there was no underlying disease, as the tests for viruses such as feline immnunodeficiency virus and feline leukemia virus were negative; neither was any known immunosuppressive therapy administered. The squamous cell carcinoma in this patient is not attributable to an aggravating factor, since the anatomical location was different and was resolved favorably with surgery. It is important to note that the feline had been living homeless before being evaluated for this mycosis, which could have influenced its immune response due to poor nutritional status.
Fonsecaea spp. has traditionally been associated with cases of chromoblastomycosis and phaeohyphomycosis in humans (Queiroz-Telles et al., 2011; Wortmann, 1995) and one case of eumycetoma (Wang et al., 2019). However, according to the literature reviewed, the present case is the first report of an eumycetoma caused by this species in a cat, with the parasitic adaptations of black grain tallus indicating this mycosis (Jensen, 2023; ).
There are reports of Fonsecaea species causing phaeohyphomycosis in domestic animals, such as Fonsecaea pedrosoi in a feline from Italy, with lesions on the nasal plane (Fondati et al., 2001), and in a dog from the United States, with pustules, erythema, and alopecia in the axillary region and ventral abdomen (Rajeev et al., 2008). In addition, there are reports of phaeohyphomycosis caused by Fonsecaea multimorphosa in a brain abscess in a cat from Australia (Najafzadeh et al., 2011).
Other genera of fungi have been reported to cause eumycetoma in wild felids, such as Curvularia sp., which has been associated with eumycetoma and phaeohyphomycosis in a captive Sumatran tiger (Panthera tigris sumatrae) in the United States (Schaff et al., 2021) and Madurella pseudomycetomatis causing eumycetoma in a captive tiger (Panthera tigris) in Italy (Orlandi et al., 2022). Therefore, it is vital to perform molecular identification when possible. In our case, this tool was not used for diagnosis.
Treatments for mycoses caused by dematiaceous fungi in cats involve a wide surgical excision of the affected area and the use of selected antifungals, based on the gender and, when possible, the species of fungus involved (Lloret et al., 2013). Among these antifungals, the latest generation of triazoles has yielded promising results, particularly itraconazole (Fondati et al., 2001) and fluconazole (Abramo et al., 2002). In one case of phaeohyphomycosis caused by Exophiala attenuata, itraconazole did not yield satisfactory results (Overy et al., 2015). There are also cases where the combination of itraconazole with terbinafine has been used, but the patient relapsed or the treatment was discontinued due to gastrointestinal side effects (Borras et al., 2022; Daly et al., 2020). In addition, regarding F. pedrosoi, there was no good response to itraconazole in a dog (Rajeev et al., 2008).
It should always be remembered that the recurrence of this pathology can be a problem (Abramo et al., 2002; Borras et al., 2022) since it also depends on the anatomical location, given that cases involving the central nervous system usually have a fatal outcome, even when the treatment prescribed is radical (Najafzadeh et al., 2011).
According to the World Health Organization, this mycosis is listed among the neglected tropical diseases (WHO, 2020) in human medicine, and eumycetoma agents are considered high-priority fungal pathogens for diagnosis, research, and development in public health actions (WHO, 2022). Regarding veterinary medicine, there are no specific recommendations concerning this fungal infection. However, as humans and domestic animals share the same environment, reporting diseases acquired from familiar sources for both animals and humans contributes to the knowledge, control, and prevention of this disease.
The authors would like to thank Paula Peña, Ericka Diez’s academic advisor when she presented this case report as her final work to obtain a degree in veterinary medicine.
The authors declare no conflict of interest.
Abramo, F., Bastelli, F., Nardoni, S., & Mancianti, F. (2002). Feline cutaneous phaeohyphomycosis due to Cladophialophora bantiana. Journal of Feline Medicine and Surgery, 4(3), 157-163. https://doi.org/10.1053/jfms.2002.0183
Arenas, R. & Torres, E. (2019). Micología médica ilustrada. (6th Ed). McGraw Hill.
Baneth, G., Petersen, C., & Sykes, J.E. (2021). Leishmaniases. In: C.E. Greene (Ed.), Infectious Diseases of the Dog and Cat (5th Ed., pp.1179-1202). Elsevier.
Barnard, N. (2013). Capítulo 5.33: Masas, nódulos e hinchazones en la piel. En A. Harvey, S. Tasker (Eds.), Manual de medicina felina (Edición en español, pp. 443-450). Lexus y Ediciones.
Barrs, V., Beczkowski, P., Tabolt, J., Hobi, S., Teoh, S., Hernandez, D., Shubitz, L., & Sandy, J. (2024). Invasive fungal infections and oomycoses in cats. Journal of Feline Medicine and Surgery, 26(1), 1-22. https://doi.org/10.1177/1098612X231219696
Bonifaz-Trujillo, A. (2020). Micología médica básica (6th Ed). McGraw Hill.
Borras, P., Messina, F., Abrantes, R., Lachini, R., Minatel, L., & Santiso, G. (2022). First Report of phaeohyphomycosis caused by Phialophora americana in a domestic cat from Argentina. Journal of Feline Medicine and Surgery Open Reports, 8(1), 1-7. https://doi.org/10.1177/20551169221077611
Calderón-Hernández, A. & Urbina-Villalobos, A. (2018). Veterinary mycoses in a tropical country. [Poster presentation]. 20th Congress of the International Society for Human and Animal Mycology. Amsterdam, The Netherlands. Abstract, Med. Mycol. 56: S1-S159. https://doi.org/10.1093/mmy/myy036
Daly, J., Hubka, V., Kubatova, A., Gilmeno, M., & Barrs, V. (2020). Feline disseminated cutaneous phaeohyphomycosis due to Exophiala spinifera. Medical Mycology Case Reports, 27, 32-35. https://doi.org/10.1016/j.mmcr.2019.12.008
Ferguson, E. (2012). Capítulo 13: Aproximación a las dermatosis faciales. En A.P. Foster, C.S. Foil (Eds.). Manual de dermatología en pequeños animales y exóticos (2nd Ed en Español, pp. 129-141). Lexus y Ediciones.
Fondati, A., Gallo, M.G., Romano, E., & Fondevila, D. (2001). A case of feline phaeohyphomycosis due to Fonsecaea pedrosoi. Veterinary Dermatology, 12(5), 297-301. https://doi.org/10.1046/j.0959-4493.2001.00262.x
Grooters, M. (2021). 87 - Miscellaneous Fungal Diseases. In: J.E. Sykes (Ed.) Greene’s Infectious Diseases of the Dog and Cat (5th Ed, pp. 1094-1104). W.B. Saunders.
Guevara-González, M. (2022). Pasantía en patología y microbiología en el Laboratorio de Patología de la Escuela de Medicina Veterinaria de la Universidad Nacional, Heredia, Costa Rica y Diagnóstico Albéitar S.A., San José, Costa Rica [*Licenciate Thesis, Universidad Nacional]. https://repositorio.una.ac.cr/items/5553ad8b-12f4-416d-a8ea-c713ed27fa62 *[Licenciate Degree: University degree between the Bachelor’s and the Master’s]
Guillot, J., García-Hermoso, D., Degorce, F., Deville, M., Calvie, C., Dickele, G., Delisle, F. & Chermette, R. (2004) Eumycetoma caused by Cladophialophora bantiana in a dog. Journal of Clinical Microbiology, 42(10), 4901-4903. https://doi.org/10.1128/JCM.42.10.4901-4903.2004
Guillot, J., Guérin, C. & Chermette, R. (2018). Histoplasmosis in Animals. In S. Seyedmousavi, G.S. de Hoog, J. Guillot, P.E. Verweij (Eds.). Emerging and Epizootic Fungal Infections in Animals (pp. 115-128). Springer.
Jensen, H. E. (2023). Histopathologic Diagnosis of Invasive Mycoses. CRC Press.
Lloret, A., Hartmann, K., Pennisi, M. G., Ferrer, L., Addie, D., Belák, S., Boucraut-Baralon, C., EgberinK, H., Frymus, T., Gruffydd-Jones, T., Hosie, M.J., Lutz, H., Marsilio, F., Möstl, K., Radford, A.D., Thiry, E., Truyen, U., & Horzinek, M. C. (2013). Rare opportunistic mycoses in cats: phaeohyphomycosis and hyalohyphomycosis. Journal of Feline Medicine and Surgery, 15(7), 628–630. https://doi.org/10.1177/1098612x13489227
Loyd, K. A. T, Hernandez S. M., Abernathy, K. J., Shock B. C., M. S., & Marshall, G. J. (2013). Risk behaviours exhibited by free-roaming cats in a suburban US town. Veterinary Record, 173(12), 295. https://doi.org/10.1136/vr.101222
Najafzadeh, M. J., Vicente, V. A., Sun, J., Meis, J. F., & de Hoog, G.S. (2011). Fonsecaea multimorphosa sp. nov, a new species of Chaetothyriales isolated from a feline cerebral abscess. Fungal Biology, 115(10), 1066-1076. https://doi.org/10.1016/j.funbio.2011.06.007
Orlandi, M., Giglia, G., Danesi, P., Laricchiuta, P., & Abramo, F. (2022). Eumycetoma caused by Madurella pseudomycetomatis in a captive tiger (Panthera tigris). Journal of Fungi, 8(12), 1289. https://doi.org/10.3390/jof8121289
Overall, K. L. (2013). Manual of Clinical Behavioral Medicine for Dogs and Cats. Mosby.
Overy, D. P., Martin, C., Muckle, A., Lund, L., Wood, J., & Hanna, P. (2015). Cutaneous phaeohyphomycosis caused by Exophiala attenuata in a domestic cat. Mycopathologia, 180(3-4), 281–287. https://doi.org/10.1007/s11046-015-9909-y
Pohlman, L. M. & Chengappa, M. M. (2022). 45 - Agents of subcutaneous mycoses. In: S. McVey, M. Kennedy, M.M. Chengappa, R. Wilkes (Eds.) Veterinary Microbiology (4th Ed., pp. 425-432). John Wiley & Sons, Inc.
Queiroz-Telles, F., Nucci, M., Colombo, A. L., Tobón, A., & Restrepo, A. (2011). Mycoses of implantation in Latin America: an overview of epidemiology, clinical manifestations, diagnosis and treatment. Medical Mycology, 49(3), 225–236. https://doi.org/10.3109/13693786.2010.539631
Rajeev, S., Clifton, G., Watson, C., & Miller, D. (2008). Fonsecaea pedrosoi skin infection in a dog. Journal of Diagnostic Investigation, 20(1), 379–381. https://doi.org/10.1177/104063870802000324
Rodrigues, M. L. & Albuquerque, P. C. (2018). Searching for a change: The need for increased support for public health and research on fungal diseases. PLoS Neglected Tropical Diseases, 12(6), e0006479. https://doi.org/10.1371/journal.pntd.0006479
Rodrigues, A. M., de Hoog, G. S. & de Camargo, Z.P. (2018). Feline sporotrichosis. In: S. Seyedmousavi, G. S. de Hoog, J. Guillot, & P. E. Verweij (Eds.). Emerging and Epizootic Fungal Infections in Animals (pp. 199-231). Springer.
Seyedmousavi, S., Guillot, J. & de Hoog, G. S. (2013). Phaeohyphomycoses, emerging opportunistic diseases in animals. Clinical Microbiology Reviews, 26(1), 19 –35. https://doi.org/10.1128/CMR.00065-12
Seyedmousavi, S., Bosco, S. M. G., de Hoog, S., Ebel, F., Elad, D., Gomes, R. R., Jacobsen, I. D., Jensen, H. E., Martel, A., Mignon, B., Pasmans, F., Piecková, E., Rodrigues, A. M., Singh, K., Vicente, V. A., Wibbelt, G., Wiederhold, N. P., & Guillot, J. (2018). Fungal infections in animals: a patchwork of different situations. Medical Mycology 56(S1), S165–S187. https://doi.org/10.1093/mmy/myx104
Schaff, A. R., Ferguson, S., Phair, K., Ferris, R., & Goe, A. (2021). Eumycetoma and disseminated phaeohyphomycosis in a Sumatran tiger. Journal of Veterinary Diagnostic Investigation, 33(6), 1197–1201. https://doi.org/10.1177/10406387211038920
Singh, K., Ilkit, M., Shokohi, T., Tolooe, A., Malik, R., & Seyedmousavi, S. (2018). Cryptococcosis: emergence of Cryptococcus gattii in animals and zoonotic potential. In: S. Seyedmousavi, G. S. de Hoog, J. Guillot, P. E. Verweij (Eds.). Emerging and Epizootic Fungal Infections in Animals (pp. 249-287). Springer.
Solano-Barquero, A., Estrada, A., Medaglia, A., Montenegro, V. M., & Rojas, A. (2022). Emerging Lagochilascaris minor infections in domestic cats from Costa Rica: A zoonotic threat for the region. Veterinary Parasitology: Regional Studies and Reports, 36, 100797. https://doi.org/10.1016/j.vprsr.2022.100797
Sykes, J. E. (2021). Chapter 90: Protothecosis and chlorellosis. In J. E. Sykes (Ed.) Greene’s Infectious Diseases of the Dog and Cat (5th Ed, pp. 1126-1134). W.B. Saunders.
Wang, R., Yao, X. & Li, R. (2019). Mycetoma in China: a case report and review of the literature. Mycopathologia 184, 327–334. https://doi.org/10.1007/s11046-019-00324-z
Westblade, L. F, Burd, E. M., Lockhart, S. R., & Procop, G. W. (2023). Larone’s Medically Important Fungi: A Guide to Identification (7th Ed). John Wiley & Sons, Inc.
World Health Organization. (2020). Ending the neglect to attain the Sustainable Development Goals: a road map for neglected tropical diseases 2021–2030. World Health Organization. https://www.who.int/publications/i/item/9789240010352
World Health Organization. (2022). WHO fungal priority pathogens list to guide research, development and public health action. World Health Organization. https://www.who.int/publications/i/item/9789240060241
Wortman, P. D. (1995). Concurrent chromoblastomycosis caused by Fonsecaea pedrosoi and actinomycetoma caused by Nocardia brasiliensis. Journal of the American Academy of Dermatology, 32(2), 390-392. https://doi.org/10.1016/0190-9622(95)90412-3

Licencia Creative Commons Atribución-No-Comercial